In less than a month, South Africa will start rolling out the most potent HIV prevention medication the world has seen. But that alone doesn’t guarantee that HIV-negative people who need this twice-a-year injection — called lenacapavir (LEN) — will use it. Uptake — and whether LEN contributes to lowering the country’s170 000 new yearly HIV infections— will depend on how the health department approaches those who need it and how accessible the medicine is.
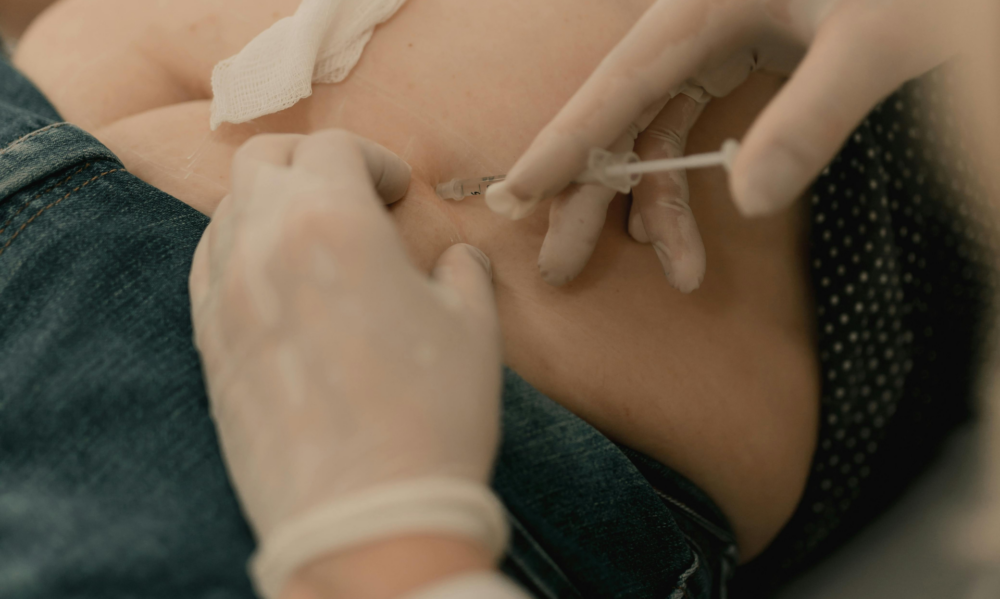
LEN isinjected into the fatty layer under the skin in someone’s tummy. The injection leaves a small supply of medicine, called a depot, under the skin that slowly releases the drug over six months. (That’s why the medicine only needs to be taken once every six months.) In a clinical trial, for which I was one of the researchers, LEN has shown perfect protection against HIV infection among teenage girls and young women between the ages of 16 and 25.
This is an important group to which LEN should be provided:about 30%of South Africa’s new HIV infections is among adolescent girls and young women, even though they constitute only8% of the population. But there’s something crucial we should remember: we’re targeting healthy, HIV-negative people. We need to treat them as such.
Read Full Article on Mail & Guardian
[paywall]
One of the key lessons I have taken from working as an HIV prevention researcher is that we have to manage people taking preventive medicine differently from patients in treatment programmes. As a medical doctor, I’ve also had to keep reminding myself of this. When people are unwell, they come to the health system.
When they are well, they don’t. They don’t want to feel like patients and they stop using services quickly if they feel judged or lectured. Healthy people are far more likely to take up preventive services when these are introduced in environments that don’t feel like hospitals.
Our role as health providers is not to hold prevention medication in the system but to make it simple, easy to get and easy to use. Because LEN is a long-acting injection and doesn’t require a young woman to agree on its use with a sexual partner, this prevention methodfits easier into many young women’s lives than condoms or once-a-day pills(a daily HIV prevention pill is stocked for free in most government clinics). I’ve seen effective tools come and go with the same limitations: daily adherence requirements, repeated clinic visits and having to negotiate use within complex relationships.
[/paywall]
All Zim News – Bringing you the latest news and updates.